CORNEAL TRANSPLANTS
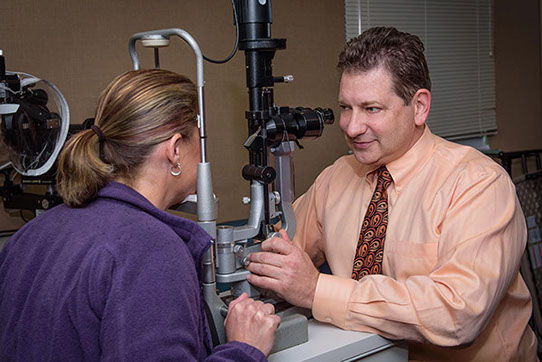
Dr. Myron Lewyckyj is our Corneal Transplant specialist, here is his approach to Corneal Transplants.
Dr. Lewyckyj graduated from Northwestern Honors Medical Program at Northwestern University where he completed his Ophthalmology residency. Dr. Lewyckyj also teaches cataract surgical techniques at Northwestern University. He is a member of the American and Indiana Academies of Ophthalmology and is certified by the American Board of Ophthalmology. Besides comprehensive ophthalmology and cataract surgery, he specializes in corneal diseases, corneal transplantation, eyelid surgery, lid lift and LASIK vision correction.
Description of corneal transplantation
Cataract consists of a clouding of the natural lens of the eye. The vast majority of us are born with a lens within our eye that is crystal clear and this typically stays clear for quite some time. The average person starts to develop some yellowing or clouding of their natural lens approximately around the age of 50, although this is highly variable.
There are some people who may be born with cataracts or develop them very early in life. The clouding and yellowing of the lens continues on a typically gradual basis throughout the years until such a point where it creates enough obstruction of vision that we consider this to be a cataract.
Cataracts may be removed in an effort to improve a person’s vision, to restore his ability to function optimally visually and in some cases for other reasons such as physical interference of the lens in the normal physiological functioning of the eye. This may be the case, for example, in certain types of glaucoma.
Types of corneal transplantation
The traditional form of corneal transplantation is called PKP or penetrating keratoplasty. This has been around for many decades in general. I have made many subtle modifications in my technique which I believe has allowed me to refine the process and limit the chances of complications and maximize the opportunity to achieve good vision. For example, I have very strict limitations on the type and age of donor tissue that I accept for corneal transplantation. I use a suturing process that encourages the cornea to take a round shape and selectively remove these sutures and use various incisions when necessary to minimize astigmatism. In cases where cataracts are concurrent, I typically prefer to do the cataract surgery subsequent to the the transplant in order to use lens implantation as a further tool minimizing the amount of eyeglass prescription afterwards. Thereby, I attempt to do whatever I can to not only have an optically clear graft, but also try to minimize the amount of eyeglass prescription that is necessary afterwards to achieve best corrected vision. When it comes to surgical technique, I have participated in developing a method of replacing the cornea which does not ever allow the eye to be fully exposed to open air and zero pressure, minimizing the chance of some of the more ominous intraoperative complications such as hemorrhage.
I am also proud to be able to offer my patients some of the newest variations of the corneal transplantation surgery. One of these is the DSEK procedure. DSEK is a partial corneal transplantation of the back layer of the cornea. It is only appropriate for people who have only an unhealthy posterior cornea, so not everyone is a candidate. It basically involves stripping away only the back layer of the cornea and replacing it with a small posterior portion of the corneal graft that is inserted through a tiny opening. The advantages of this approach are a small incision size and rapid return to physical activity. Rehabilitation of vision may also be quite rapid, sometimes on the order of several weeks instead of six months. The disadvantage of this type of procedure is that occasionally more than one follow-up procedure is necessary. The graft must be floated up on an air bubble and made to adhere the underside of the cornea. In some instances, the graft can be traumatized by this process and/or may slip off. Subsequent procedures may be needed to cause the transplant tissue to re-adhere, or replacement of the transplant may be needed. Nevertheless, this is still an excellent option for some patients
I am also proud to offer the DALK procedure (deep anterior lamellar keratoplasty) which is a partial transplantation of the anterior cornea, which may also be appropriate for some patients in certain situations where there is a disruption of only the front part of the cornea. This is especially useful where the patient has a limited ability to cooperate and avoid rubbing their eye.
As with other aspects of opthalmologic care, I firmly believe is it important to match the type of corneal transplantation procedure to the individual needs of the patient and the specifics of the particular eye being worked on.
I am happy to be able to offer a variety of methods to best suit the individual needs and specifics of a given patient and to help them choose the best pathway for them to optimal visual recovery and good sight.